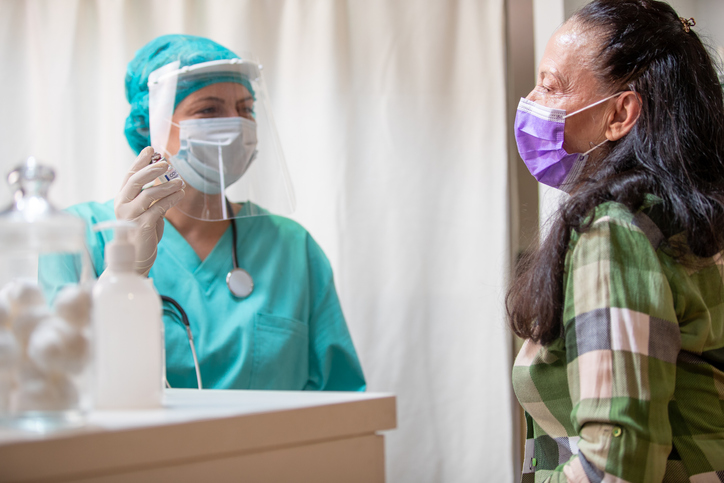
COVID-19 Vaccine: Protect Your Health
As someone with type 2 diabetes, you may already know the bad news: type 2 diabetes, especially if it’s not well managed, increases your chance for severe complications if you get COVID-19.
Now, the really, really (really!) good news we’ve waited for, we have a safe and effective vaccine for COVID-19. Did you hear that? A time when you can hug loved ones and avoid mentally measuring six feet from strangers is in sight! We’re so close to this future now that we have a proven way to help prevent this unpredictable and devastating virus that has taken so many lives and upturned millions of others.
What do I need to do?
You’ve already done so much. You’ve been diligent about managing your diabetes. You’ve been following the COVID-19 prevention playbook: Wear a mask! Wash your hands! Avoid crowds! Now it’s time to add one more, get the vaccine when it’s available to you. Everyone will still need to stick with the COVID-19 prevention playbook and keep conditions like diabetes and high blood pressure well managed to beat the virus, but you can think of getting the vaccine as your not-so-secret weapon.
Does it work?
The medical experts at the American Heart Association® (AHA) and the American Diabetes Association® (ADA) agree with scientists around the world that the COVID-19 vaccine is the most powerful tool we have to protect ourselves and our loved ones from its potential severe complications. This is the number one thing that will get us back to the life we miss.
Is it safe?
Yes, the COVID-19 vaccine is safe. Each available vaccine has gone through rigorous testing and been approved by the U.S. Food and Drug Administration (FDA). It’s safe for people of color, people with diabetes, people with a history of heart disease or stroke, and other underlying health issues such as chronic kidney disease, all of whom were part of the trials. Of course, if you have questions that pertain to a unique situation, contact your doctor’s office now to ask if you should and when you’re able to get it.
With all that’s changed over the last year, one thing has remained the same—at both the AHA and the ADA, your health is our number one priority and that one thing drives everything we do.
Glossary
Do you ever get lost when you’re talking to your doctor because you don’t know the words being used?
Sometimes your doctor or other members of your health care team may use words you aren’t familiar with or that you’ve heard but don’t quite understand. If you feel confused about something your doctor is telling you, ask for it to be explained. Even with answers, you may still feel confused or uncertain about what you need to do following your visit.
We want to help you get the most out of your visit, so we’ve pulled together some commonly used terms your doctor might use when explaining how to better manage your diabetes and risk for heart disease and stroke:
- A1C—An A1C blood test can be used to diagnose diabetes or identify prediabetes. It is also used to check how your diabetes treatment is working over time. This relatively simple blood test tells you your average blood sugar (also called blood glucose) level over the past two to three months. A higher level can tell you if you have diabetes or prediabetes and, if you have diabetes, how your treatment is working. If your A1C is higher than your targets, it raises your risk of developing complications. The goal for most adults with diabetes is an A1C less than 7%. Usually your doctor will order this test twice a year or more often, if needed.
- Albumin—Albumin is a protein made by your liver that helps keep fluid in your bloodstream, so it doesn’t leak into other tissues. It also carries various substances throughout your body, including hormones, vitamins, and enzymes. Low albumin levels may lead to fluid retention, and can indicate a problem with your liver or kidneys.
- Antihyperglycemic agents—Antihyperglycemic agents lower your blood sugar levels. They can be taken as pills or injected and are used in the treatment of type 2 diabetes. For many people metformin is the first medication prescribed. Some antihyperglycemic agents, GLP-1s and SGLT-2s, have benefits for your heart and kidneys as well.
- Blood glucose—Blood glucose, or more commonly called blood sugar, is found in the blood and is the body’s main source of energy. If you have diabetes, your body has trouble processing blood sugar. There are a variety of ways to check your blood sugar levels, which tell you if you have diabetes or how your treatment is working if you have diabetes.
- Body mass index—Body mass index (BMI) is a measure of your body weight relative to your height. BMI, along with other measurements such as waist-to-hip ratio, can be used to help decide whether a person is underweight, normal weight, overweight, or obese.
- Glomerular filtration rate (GFR)—A glomerular filtration rate is a test used to check how well your kidneys are working. Specifically, it estimates how much blood passes through the glomeruli each minute. Glomeruli are the tiny filters in the kidneys that filter waste from the blood. A blood sample is sent to a lab where the creatinine level in the blood sample is tested. Creatinine is a chemical waste product of creatine—a chemical the body makes to supply energy, mainly to the muscles.
- Hyperlipidemia—Hyperlipidemia is when the fat (triglyceride) and cholesterol (total cholesterol and/or LDL cholesterol) levels in your blood are too high.
- Hypertension (high blood pressure)—Hypertension occurs when blood flows through the blood vessels with a force greater than normal. The extra pressure can strain your heart, damage blood vessels, and increase the risk of heart attack, stroke, kidney problems, and death. The goal for most adults is less than 120/80. Your doctor will give you a target that’s right for you.
- Hypoglycemia (low blood sugar)—Hypoglycemia when your blood sugar is lower than normal (less than 70 mg/dL). Signs include if you’re hungry, nervous, shaky, sweating, dizzy, light-headed, sleepy, or confused. If left untreated, it may lead to more serious complications, like losing consciousness. Hypoglycemia is treated by eating a food that’s a source of carbohydrate that will be processed by your body quickly, such as glucose tablets or juice. Severe hypoglycemia, where a person can’t speak or swallow, is treated with glucagon—either injected or inhaled—if the person is unconscious or unable to swallow.
- Hyperglycemia (high blood sugar)—Hyperglycemia is when your blood sugar levels are above normal.
- Insulin—Insulin is a hormone produced by the pancreas that helps your body use glucose for energy. If your body cannot make enough insulin and other medications aren’t helping you reach your blood glucose targets, insulin may be prescribed. Insulin is taken by injection or through use of an insulin pump.
- Titration—The amount of insulin a person with diabetes needs to take based on a variety of factors such as mealtime carbohydrate load, blood sugar levels, and exercise. For people starting insulin treatment, the initial dose is often relatively small and is increased over the course of the ensuing few days and weeks.
- Urine albumin-to-creatinine ratio (UACR)—Your urine albumin-to-creatinine ratio (UACR) shows whether you have albumin in your urine. Albumin is a type of protein that’s normally found in the blood, not in your urine. People with a high amount of albumin in their urine are at an increased risk of having chronic kidney disease which could progress to kidney failure. The UACR screening is a simple urine test that’s part of a routine exam.
Remember, it’s OK to ask your doctor to explain something in a different way. Have a question? Just ask. Your health care team is there for you.
3 Kidney-Related Questions to Ask Your Doctor if You Have Diabetes
Communication Is Important
Health care is a team effort and you play an important role. You can make sure you get the best possible care by talking with your doctor and asking questions.
Keep reading to learn why asking your doctor the right questions is an important part of your diabetes management.

How Are the Heart, Kidneys and Diabetes Connected?
Your kidneys are powerful filters that remove toxins from your blood through your blood vessels (arteries, veins, and capillaries)—which are part of your cardiovascular system.
Type 2 diabetes can put a lot of stress on both your heart and in your kidneys. If you have type 2 diabetes and develop kidney disease, you’re at 3x higher risk of dying from a cardiovascular event like a heart attack or stroke. To stay healthy, it’s important for you and your doctor to manage your risk of both.
Asking questions about your diagnoses, treatments and medications is one of the best ways to lower your risk for diabetes-related complications like heart disease, stroke and kidney disease.

Preparing for Your Appointment
You can prepare for your appointment by thinking about what you want to do during your next visit.
Do you want to:
- Start or change a medicine?
- Get medical tests?
- Talk about lifestyle changes and treatment options?
Write down your questions in your phone or a notepad to help you feel prepared and less rushed during your appointment.
During Your Appointment To get the most from your visit, tell the nurse or person at the front desk that you have questions for your doctor. If your doctor does not ask if you have questions, ask your doctor when the best time would be to ask them. Start by asking the ones that are most important to you.

3 Kidney-Related Questions to Ask Your Doctor if You Have Diabetes
Asking questions is important but so is making sure you hear—and understand—the answers you get. Take notes or ask to record them on your phone or another device. If you want to bring someone to your appointment to help you understand and remember what you heard, call and ask the doctor’s office ahead of time if that’s okay. If you don’t understand or are confused, ask your doctor to explain the answer again.
3 Questions to Prevent Kidney Disease
- Have I received my annual urine albumin-creatinine ratio (UACR) screening?
- What signs or symptoms of kidney disease should I be aware of?
- How do I take care of my kidneys and reduce my risk for heart disease and stroke?
It is very important to understand the next steps your doctor recommends. Ask more questions, if you need to, and make sure you know what your doctor wants you to do. Asking for written instructions, brochures, videos, or websites may also help you learn more.

Understand the Answers and Next Steps
After you meet with your doctor, you will need to follow the instructions to keep your health on track. You may need to follow up on your care and call your doctor. Call your doctor if:
- You have side effects or problems with your medications.
- Your symptoms get worse after your appointment.
- You get new prescriptions from other members of your health care team or start taking any over-the-counter medicines.
- You need the results of any tests you’ve had. Don’t assume that no news is good news—be proactive.
- You don’t understand your test results.
Asking questions can help your health care team learn more about you. Their answers can help you make better decisions, receive a higher level of care, prevent symptomless diabetes-related complications like kidney disease and feel better about the care you receive.
If you have diabetes, good communication with your health care team is key. There are questions you can ask to reduce your risk of kidney disease, heart disease and stroke. Talk to your doctor, be curious and, most importantly, make sure you understand the answers.
5 Steps to Preventing Kidney Disease Before It Starts
You may have heard if you have type 2 diabetes, you have an increased risk of kidney disease, often called chronic kidney disease or CKD. Here, we explain what you need to know about preventing kidney disease, how your heart and kidney health is connected and the role of regular screenings. Read on to learn how to take care of your kidneys and lower the risk for heart disease when living with diabetes.
What Causes Kidney Failure?
To understand what causes kidney failure, it’s important to understand how healthy kidneys function and what purpose they serve.
The kidneys are amazing organs that work hard to filter our body’s blood. With thousands of tiny blood vessels, our kidneys act as a full-body filtration system. They separate waste products from essential substances like protein and red blood cells in the body.
Kidney failure occurs when this system breaks down and useful bodily substances, like protein, are unintentionally expelled. Protein is necessary for the body’s tissues and organs—and we need it to survive. When the filtering system is in the early stages of protein loss, it is called microalbuminuria. More extensive breakdown is known as macroalbuminuria.
Thankfully, you can test kidney function to find out about problems early—and make changes to prevent kidney disease with a simple screening.
How Are the Heart, Kidneys and Diabetes Connected?
Your kidneys are part of your cardiovascular system and type 2 diabetes can put a lot of stress on both your heart and your kidneys. To stay healthy, it’s important for you and your doctor to keep tabs on your risk for problems in both your heart and kidneys and to take care of problems you may have.
What Is a UACR Screening?
Our bodies need protein to build muscle, fix tissue and fight infection. But it should be in the blood, not urine, where protein is lost if you have kidney damage. People with a high amount of protein (albumin) in their urine have an increased risk of kidney disease. In these cases, dialysis may be needed to survive. The urine albumin-to-creatinine ratio (UACR) is a simple test that shows whether albumin is present in the urine.
A UACR test can be an early sign of kidney damage and should be part of your annual screenings if you are a person with type 2 diabetes.
What are the Symptoms of CKD?
If you have had diabetes for many years, you could have kidney damage and not even know. High blood glucose (blood sugar), high blood pressure and diabetes-related complications contribute to kidney disease.
Unfortunately, recognizing early-stage kidney disease by checking for symptoms is usually not possible. This is because our kidneys will overwork themselves to make up for the early damage, and you may not have symptoms until nearly all function is gone. Any symptoms you may have wouldn’t make you think it’s kidney disease. This is why it is so important to see your doctor regularly and get checked, annually.
Does Everyone With Diabetes Develop Kidney Disease?
Many people ask if being diagnosed with diabetes automatically means they’ll struggle with kidney disease, and the answer is no. Factors that can influence kidney disease development include genetics, long-term high blood glucose and high blood pressure.
It is important to see your doctor regularly and maintain an ongoing conversation about your health. The better you’re able to keep your diabetes and blood pressure under control, the lower your chance of getting kidney disease. When you schedule a UACR screening, your doctor will check your blood pressure, your urine protein ratios and talk with you about lifestyle prevention steps.
What can I do for Prevention?
1. Understand risk factors
When you’re living with diabetes, high blood glucose levels can cause your kidneys to work harder. Over time, kidney failure is more likely to occur.

2. Be Proactive
If you develop kidney disease, it is likely that you’ll have little to no symptoms until almost all function is gone. Have a discussion with your doctor about how to protect your heart and kidneys. Regular UACR screenings are key to early detection. When kidney disease is diagnosed early, several treatments may keep it from getting worse.

3. Manage your blood sugar and blood pressure to keep them in your target range
Blood sugar management can reduce the risk of early-stage kidney failure by one-third and may reduce the risk of early stages of kidney disease to more severe kidney disease by half. Some studies have shown tight management can even reverse the early stages.

4. Talk to your your health care team about any special needs you may have
Some treatments used may limit certain types of foods you eat. Always talk with your health care team before changing your diet.

5. Get regular screenings
Ask your doctor for a UACR screening once a year if they haven’t scheduled one. This simple urine test is often overlooked but can mean the difference between staying healthy and avoiding dialysis. Your doctor can check your blood pressure, eGFR (estimated glomerular filtration rate), urine protein ratios and talk with you about lifestyle prevention steps.
If you have diabetes, there are simple, preventative steps you can take to lower your risk of heart disease. Talk to your doctor about how to keep your heart healthy and about getting regular UACR screenings to help you understand the health of your kidneys.
Managing Your Diabetes Starts with Education
Get the latest information and the support you need, all in one easy place.
Managing your diabetes starts with learning about it and having your questions answered, but it can be tough to gain the skills you need — especially if you haven’t been to an education program. Now, you can find the support and information you need to live well with diabetes — and we have everything you need, all in one easy place.
The Easy Way to Manage Your Diabetes
American Diabetes Association® Recognized Education Programs are ready to work with you to find practical solutions that fit your personal needs. Learn how to manage the link between diabetes and heart disease so that you can reduce your risk of heart attack and stroke.
Diabetes Self-Management Education and Support (DSMES) Services
If you have type 2 diabetes, Diabetes Self-Management Education and Support (DSMES) Services will help you navigate your diabetes journey. Here, you’ll find the direction, resources and support you need to succeed.
This program is designed to support you and help you become more confident and empowered as you learn to make your journey easier than ever. Work hand in hand with a diabetes educator during a series of personalized sessions to understand how to manage your diabetes. DSMES is a cost-effective tool, proven to improve health behaviors and health outcomes for people with diabetes. And here’s some good news: If your doctor refers you to a program, most insurance plans will often cover the cost!
Ready to get started?
Here are three easy steps you can take to empower your diabetes journey:
- Visit our site to find a program near you.
When you visit our site, you’ll be able to answer questions so that you can find practical solutions that fit your individual needs. - Ask your doctor for a referral.
Wondering when the right time is to request a referral from your doctor?If you’ve never taken part in a diabetes education program or you’re newly diagnosed, requesting a referral from your doctor is a great place to start. Managing diabetes can be extra tough during times of transition, too. If you’ve recently experienced a change in your health or living situation, have started a new medication, received new insurance coverage or have had changes in access to food or money, we recommend asking for a referral. - Start getting the support you need.
If you have diabetes, there is a lot you can do. Talk to your doctor about your next steps and explore the resources we’ve created just for you.
Answers That Matter
We know how important it is to have your personal concerns heard and addressed. That’s why we created our monthly Ask the Experts series. Designed to help people with diabetes tackle commonly faced issues, this Q&A series provides a community where individuals can ask questions of our experts and hear from others who share similar experiences — all for free. Get your questions ready; answers are on their way.
Living with Type 2 Diabetes
Created for those recently diagnosed with type 2 diabetes, the Living With Type 2 Diabetes program offers participants an opportunity to learn about diabetes and diabetes management gradually over a 12-month period. See what this free program — available in English and Spanish — provides.
Diabetes Food Hub™
Browse tasty recipes, create a shopping list and meal plan all in one place! Check out our healthy eating blog for the latest nutrition knowledge and meal prepping tips and tricks, and create an account for your free, all-access pass to hundreds of recipes and more. ¡Recibas en español Tambien!
Heart Disease and Stroke
The Relationship Between Diabetes, Heart Disease and Stroke
Did you know that T2D is linked to an increased risk of heart disease and stroke? In fact, adults with diabetes are twice as likely to have a heart attack or stroke than people without diabetes, even if their diabetes is well managed. Learn more about the connection below!
Diabetes and heart disease put you at higher risk of complications if you get COVID-19. There are basic steps anyone can take to reduce their risk of getting the virus. Stay vigilant. If you have diabetes and/or heart disease and get COVID-19, you might experience more severe symptoms or serious complications.

Overall, there’s a lot you can do to reduce your risks of heart disease and stroke.
First, talk to your health care provider to better understand your condition and what you can do to stay healthy. With COVID-19, many health care providers are willing to communicate via phone, email or a secure patient portal.
“Diabetes is more complicated than most chronic diseases, so it’s important to be proactive and work with your health care team to learn all you can about how to manage it,” said Robert Eckel, M.D., Professor Emeritus at the University of Colorado Anschutz Medical Campus and former president of the American Heart Association® (AHA).

Reducing your risk starts with making sure your diabetes is well controlled. Work with your health care team to set goals that can get your health on track.
When your blood sugar (blood glucose) is high (called hyperglycemia), it can damage blood vessels over time. Excess cholesterol also makes your blood vessels stiff when there is a build-up of a fatty substance called plaque, affecting blood flow.
Many people with diabetes also have other conditions—including extra weight, high blood pressure and high triglycerides—that increase the risk for heart disease. Work with your health care team, you may need a combination of lifestyle changes and medication to manage those factors.
Stay in contact with your health care team about your progress and make sure you don’t miss your appointments. Be prepared with questions. Talk about steps you can take before your next appointment and how to track your progress.
Many people with diabetes need to take one or more medications to manage their diabetes. Make sure you take all your medications as prescribed. If you are running into challenges or if the side effects are difficult to manage, talk with your doctor about alternatives.

Other Ways to Manage Diabetes, Heart Disease and Stroke
If you use tobacco, stop. Stick your eating plan or work with your health care team for specifics about what’s right for you.
Get your heart rate up. Aim for at least 150 minutes each week of moderate aerobic activity like a brisk walk. This can be split up into 30 minutes of activity every day and doesn’t need to be all at once. If 30 minutes is too much, try taking 10-minute walks three times a day to reach your goal.
With an increased risk for stroke, it’s important that you and those around you recognize the common symptoms of a stroke. F.A.S.T. is an easy way to remember that if your face is drooping or you experience arm weakness or speech difficulty, it’s time to call 911 and get immediate medical attention.
Most of all, stay positive. There are millions of people with diabetes leading healthy lives and you can be one of them.
Learn more about the link between diabetes and heart disease and stroke at KnowDiabetesByHeart.org.
For More Information:
Types of Diabetes
Did you know there’s more than one type of diabetes? Most people have heard of type 2, type 1 and gestational diabetes; however, there are additional forms of the disease, such as latent autoimmune diabetes (LADA), and maturity-onset diabetes of the young (MODY).
Here, we’ll discuss the most common types of diabetes and the best practices to treat each one.
Types of diabetes PDF (Spanish)
Type 2
This is the most common form of the disease and accounts for nearly 90-95% of cases. In this instance, your body still produces insulin, but does not make enough or use it efficiently. The best treatment options are eating a balanced diet; starting or increasing physical activity; regularly monitoring your blood glucose and taking medication prescribed by your doctor, if needed. Most often found in middle-aged and older adults, younger people can also be diagnosed with type 2 diabetes.
Type 1
Accounting for about 5% of diabetes cases, type 1 diabetes often begins in childhood, but can occur at any age. In type 1 diabetes, the body produces little or no insulin. Unlike type 2 diabetes where taking insulin may or may not be part of a treatment plan, people living with type 1 diabetes must use insulin to survive.
People with type 1 diabetes manage their diabetes with healthy eating and physical activity, along with using insulin and carefully monitoring blood glucose levels.
Gestational Diabetes
Pregnancy is beautiful and can also be taxing on the body. Sometimes, when women aren’t able to produce enough or properly use insulin, they’re diagnosed with diabetes during their pregnancy; this is known as gestational diabetes. The onset of this type of diabetes usually happens around the 24-week period, and the treatment plan generally includes a special meal plan, scheduled light physical activity, regular blood sugar monitoring, and may also require insulin.
Who is most likely at risk?
Now that we’ve discussed the various types of diabetes, let’s take a closer look at the populations, personal habits and family history of those most likely to encounter the disease.
You’re more likely to develop type 2 diabetes if you’re:
- Hispanic or Latino
- Black or African American
- American Indian
- Asian (especially South Asian)
- Pacific Islander
Additional factors for type 2 diabetes:
It’s a lot of information, but there’s a lot you can do.
Did you know adults with diabetes are two times more likely to experience a stroke or develop heart disease? That’s why keeping your heart healthy and your blood pressure in check (plus other numbers) are such important priorities.
And, if you are someone living with diabetes or serving as a caregiver for someone else, it may feel overwhelming— but you’re not alone. The first course of action is to establish a treatment plan with your doctor’s help. And while you’re there, don’t forget to discuss how a medication plan can help reduce the risk of developing cardiovascular disease.
We’re here to help by providing the most up-to-date information and resources available to combat all types of disease. Yes, diabetes is a lot … but there is so much you can do to manage the disease and live a happier, healthier life.




